PANDAS and Sydenham’s chorea
PANDAS AND SYDENHAM’S CHOREA
PANDAS is not the first neuropsychiatric disorder to be associated with Group A streptococcal infections and autoimmunity. Sydenham’s chorea, a neurologic manifestation of an autoimmune response to a streptococcal infection, was first identified in the 1800s as well as the relationship to rheumatic fever and choreiform movements also known as Saint Vitus’s dance.* Sydenham’s chorea is believed to be a medical model for PANDAS as they both share considerable overlap in their clinical presentation and immunology.
* Vale, T. C. and F. Cardoso (2015). “Chorea: A Journey through History.” Tremor Other Hyperkinet Mov (N Y) 5.
In the 1990s, the NIH identified a subgroup of children who presented with a sudden onset of OCD and/or tics in association with a recent Group A streptococcal infection. However, these patients did not meet the criteria for Sydenham’s chorea 1 and were subsequently classified as PANDAS – Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections.
“PANDAS may be thought of as ‘rheumatic fever’ of the brain. And just as Sydenham’s chorea gives you abnormal movements, PANDAS gives you abnormal thoughts and behaviors.” 2
PANDAS vs. non-PANDAS patients
Some MRI studies have shown that children with PANDAS have neuroanatomical differences when compared to non-PANDAS patients. They have significantly larger basal ganglia structures on MRI than healthy age-matched controls. 5 And, there is evidence that the basal ganglia, in particular dopamine receptors, are targeted by autoantibodies triggered by Group A streptococcal infections. 6,7,8,9,10
The basal ganglia is responsible for a variety of biological functions including: control of voluntary motor movements, procedural learning, eye movements, cognition, emotion and routine behaviors.
Immunological mechanism of Sydenham’s chorea
Sydenham chorea is a neuropsychiatric consequence of a group-A streptococcal infection, and is associated with autoantibodies directed against the basal ganglia of the brain. 19
Studies show children who meet the PANDAS criteria have higher levels of circulating antibodies targeting the caudate and putamen (parts of the basal ganglia) neuronal surface antigens in the midbrain, compared to children with Tourette’s syndrome or other tic disorders. 7,8
The increase in the size of the caudate and putamen suggests there’s autoimmune inflammation in these areas.
Studies show children who meet the PANDAS criteria have higher levels of circulating antibodies targeting the caudate and putamen neuronal surface antigens in the midbrain, compared to children with Tourette’s syndrome or other tic disorders. 7,8
The increase in the size of the caudate and putamen suggests there’s an ongoing autoimmune inflammation in these areas.
PANDAS has also been reported in children with an existing tic disorder or Tourette’s syndrome. In this scenario, the baseline frequency of the child’s tics may markedly increase when the child has a strep infection and return to baseline rates after antibiotic treatment. 11-16
Specific antibodies against neuronal surface glycolytic enzymes, lysoganglioside and N-acetyl-β-D-glucosamine, are found to be in higher concentrations and more active in children with tics compared to those children with only Group A streptococcal pharyngitis and without tics. 17,18
Cunningham Panel™ antibody tests successfully identify acute illness in Sydenham chorea and PANDAS patients.
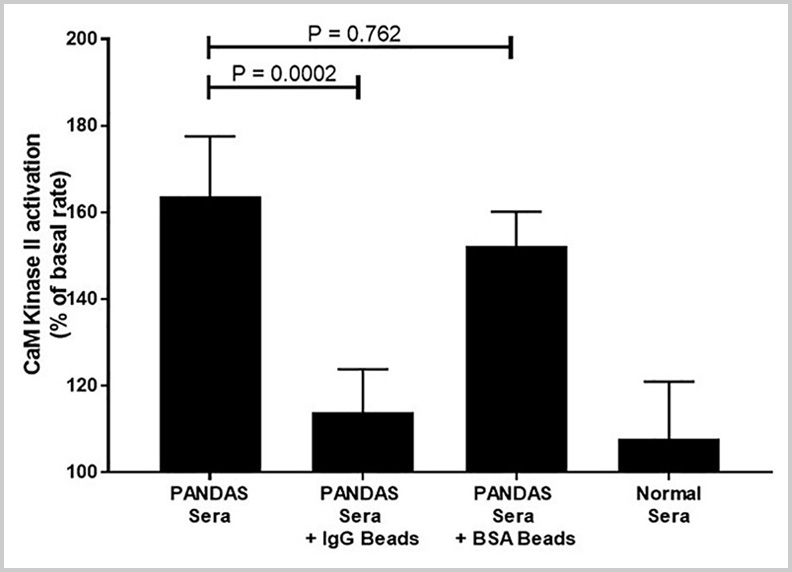
Autoantibody Biomarkers for Basal Ganglia Encephalitis in Sydenham Chorea and Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal Infections (PANDAS)
Author’s Take:
- Swedo SE, Rapoport JL, Cheslow DL, et al. High prevalence of obsessive-compulsive symptoms in patients with Sydenham’s chorea. The American Journal of Psychiatry. Feb 1989;146(2):246-249.
- Swedo SE, Leonard HL, Kiessling LS. Speculations on antineuronal antibody-mediated neuropsychiatric disorders of childhood. Pediatrics. Feb 1994;93(2):323-326.
- Radio interview with Dr. Susan Swedo, magic983.com, 10/12/2014.
- Swedo SE, Leonard HL, Kiessling LS. Speculations on antineuronal antibody-mediated neuropsychiatric disorders of childhood. Pediatrics. Feb 1994;93(2):323-326.
- Giedd JN, Rapoport JL, Garvey MA, Perlmutter S, Swedo SE. MRI assessment of children with obsessive-compulsive disorder or tics associated with streptococcal infection. The American Journal of Psychiatry. Feb 2000;157(2):281-283.
- Brimberg L, Benhar I, Mascaro-Blanco A, et al. Behavioral, pharmacological, and immunological abnormalities after streptococcal exposure: a novel rat model of Sydenham chorea and related neuropsychiatric disorders. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology. Aug 2012;37(9):2076-2087.
- Pavone P, Bianchini R, Parano E, et al. Anti-brain antibodies in PANDAS versus uncomplicated streptococcal infection. Pediatric neurology. Feb 2004;30(2):107-110.
- Church AJ, Dale RC, Lees AJ, Giovannoni G, Robertson MM. Tourette’s syndrome: a cross sectional study to examine the PANDAS hypothesis. Journal of neurology, neurosurgery, and psychiatry. May 2003;74(5):602-607.
- Dale RC, Heyman I, Giovannoni G, Church AW. Incidence of anti-brain antibodies in children with obsessive-compulsive disorder. The British Journal of Psychiatry : the journal of mental science. Oct 2005;187:314-319.
- Dale RC, Merheb V, Pillai S, et al. Antibodies to surface dopamine-2 receptor in autoimmune movement and psychiatric disorders. Brain : a journal of neurology. Nov 2012;135(Pt 11):3453-3468.
- Cohen DJ, Leckman JF. Developmental psychopathology and neurobiology of Tourette’s syndrome. Journal of the American Academy of Child and Adolescent Psychiatry. Jan 1994;33(1):2-15.
- Cohen DJ, Leckman JF, Pauls D. Neuropsychiatric disorders of childhood: Tourette’s syndrome as a model. Acta Paediatr Suppl. Jul 1997;422:106-111.
- Cohen DJ, Leckman JF. Tourette’s syndrome. JAMA : the Journal of the American Medical Association. Apr 3 1991;265(13):1738.
- Findley DB, Leckman JF, Katsovich L, et al. Development of the Yale Children’s Global Stress Index (YCGSI) and its application in children and adolescents with Tourette’s syndrome and obsessive-compulsive disorder. Journal of the American Academy of Child and Adolescent Psychiatry. Apr 2003;42(4):450-457.
- Murphy TK, Sajid M, Soto O, et al. Detecting pediatric autoimmune neuropsychiatric disorders associated with streptococcus in children with obsessive-compulsive disorder and tics. Biological psychiatry. Jan 1 2004;55(1):61-68.
- Leslie DL, Kozma L, Martin A, et al. Neuropsychiatric disorders associated with streptococcal infection: a case-control study among privately insured children. Journal of the American Academy of Child and Adolescent Psychiatry. Oct 2008;47(10):1166-1172.
- Findley DB, Leckman JF, Katsovich L, et al. Development of the Yale Children’s Global Stress Index (YCGSI) and its application in children and adolescents with Tourette’s syndrome and obsessive-compulsive disorder. Journal of the American Academy of Child and Adolescent Psychiatry. Apr 2003;42(4):450-457.
- Murphy TK, Sajid M, Soto O, et al. Detecting pediatric autoimmune neuropsychiatric disorders associated with streptococcus in children with obsessive-compulsive disorder and tics. Biological psychiatry. Jan 1 2004;55(1):61-68.
- Chain Jennifer L., Alvarez Kathy, Mascaro-Blanco Adita, Reim Sean, Bentley Rebecca, Hommer Rebecca, Grant Paul, Leckman James F., Kawikova Ivana, Williams Kyle, Stoner Julie A., Swedo Susan E., Cunningham Madeleine W. “Autoantibody Biomarkers for Basal Ganglia Encephalitis in Sydenham Chorea and Pediatric Autoimmune Neuropsychiatric Disorder Associated With Streptococcal Infections.” Frontiers In Psychiatry, vol. 11, 2020, p. 564., doi: https://www.frontiersin.org/article/10.3389/fpsyt.2020.00564
Learn More About PANS & Pandas and The Cunningham Panel™

PANS: Diagnosis and Treatment

PANDAS & PANS Patient Stories