Lyme disease and the immune system: elevated neuronal autoantibodies associated with persistent symptoms
Cunningham Panel™ results indicate Lyme disease may trigger autoimmune dysfunction

This newly published study, which examined Lyme disease and the immune system, illustrates molecular mimicry targeting neural tissue after Borrelia burgdorferi (Bb) infection. The authors test the hypothesis that autoantibodies produced in patients with early Lyme disease and Post-Treatment Lyme Symptoms (PTLS) cross-react with neuronal antigens and potentially lead to Lyme disease sequelae. The authors conclude that patients with Lyme disease have a greater frequency of certain anti-neuronal autoantibodies and functional neuronal activation compared to community controls without a history of Lyme disease 1.
Elevated autoantibody results measured by the Cunningham Panel in this study included anti-lysoganglioside GM1, anti-D1R, and anti-D2R. Elevated CaMKII activation suggests that antineuronal antibodies have functional significance.
“A heightened immunological response triggered by repeated infection with Bb may increase the risk for neurologic and neuropsychiatric symptoms among patients with previously treated LD (Lyme disease).”
This study examined 179 serum samples for the presence of Lyme disease and immune system reactivity. Patients were assigned to one of four groups:
- Patients with first episode of LD with Erythema Migrans (EM) rash
- Patients re-infected with Bb (recent episode of LD with EM rash and previously treated LD)
- Patients with LD diagnosis at least 6 months prior to the study who reported ongoing symptoms (fatigue, pain, cognitive problems) despite antibiotic treatment (PTLS)
- Healthy controls with no history of LD
Highlights:
- “Significantly higher titers” for anti- lysoganglioside GM1, anti-D1R and anti-tubulin were found in re-infected patients (EM + Prior LD). In fact, for this group, anti-lysoganglioside GM1 titers were 4 times higher (640 vs 160), while anti-D1R (8000 vs 4000) and anti-tubulin (3000 vs 1500) were 2 times higher than controls. Additionally, the CaMKII assay was significantly elevated in this group, indicating functional significance.
- The PTLS group had considerably higher titers of anti-lysoganglioside GM1 antibodies compared to controls (320 vs 160).”
- These observations raise the possibility that “elevated anti-lysoganglioside antibody levels may play a role in symptom persistence”, which suggests an immune priming effect of repeated infection, and also raises the possibility that a noninfectious immune-mediated process may be inducing disease.
- The authors suggest that neurologic and neuropsychiatric symptoms may emerge, “as a result of elevated autoantibodies against anti-lysoganglioside GM1 … and against the dopamine 1 receptor, both leading to activation of CaMKII in neuronal cells.”
Additional Research:
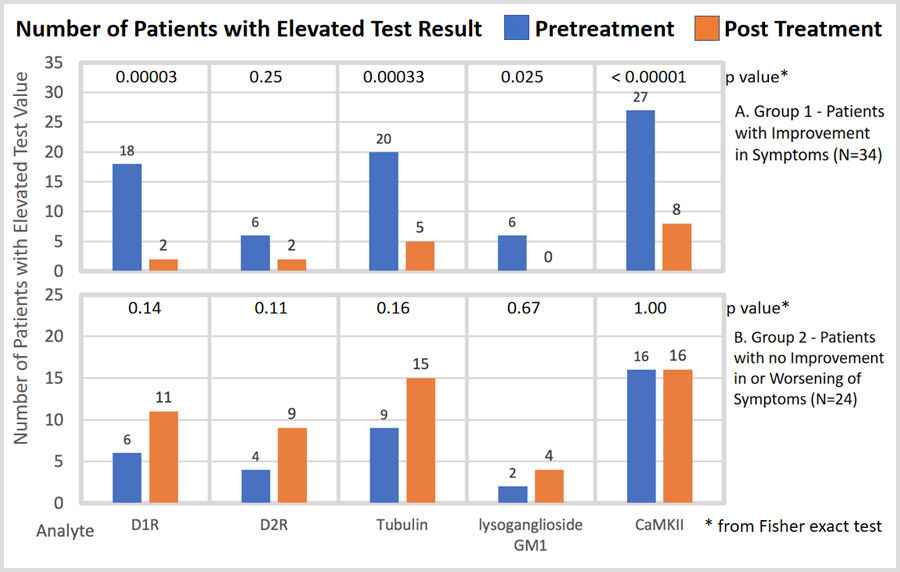
This newly published study examined whether changes in patient pre- and post-treatment symptoms correlated with changes in anti-neuronal autoantibody titers and the neuronal cell stimulation assay in the Cunningham Panel in patients with Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal Infection (PANDAS), and Pediatric Acute-onset Neuropsychiatric Syndrome (PANS). 2.
Clinicians: Schedule a Personal Phone Consultation with our Clinical Staff
Learn more about how the Cunningham Panel™ of tests can assist you in diagnosing treatable autoimmune encephalopathies characterized by abnormal neuropsychiatric behaviors. Schedule your personal phone consultation with a Moleculera Labs clinical staff member by completing the form below.
1 Brian A. Fallon, Barbara Strobino, Sean Reim, Julie Stoner, Madeleine W. Cunningham, Anti-lysoganglioside and other anti-neuronal autoantibodies in post-treatment Lyme Disease and Erythema Migrans after repeat infection, Brain, Behavior, & Immunity – Health, 2020,100015,ISSN 2666-3546, https://doi.org/10.1016/j.bbih.2019.100015
2 Craig Shimasaki, Richard E. Frye, Rosario Trifiletti, Michael Cooperstock, Gary Kaplan, Isaac Melamed, Rosalie Greenberg, Amiram Katz, Eric Fier, David Kem, David Traver, Tania Dempsey, M. Elizabeth Latimer, Amy Cross, Joshua P. Dunn, Rebecca Bentley, Kathy Alvarez, Sean Reim, James Appleman. Evaluation of the Cunningham Panel™ in pediatric autoimmune neuropsychiatric disorder associated with streptococcal infection (PANDAS) and pediatric acute-onset neuropsychiatric syndrome (PANS): Changes in antineuronal antibody titers parallel changes in patient symptoms. Journal of Neuroimmunology, In Press-15 February 2020.Online ahead of print https://www.jni-journal.com/article/S0165-5728(19)30352-2/fulltext