An atypical presentation of Pediatric Acute Neuropsychiatric Syndrome responding to plasmapheresis treatment
Case review: Dr. Shimasaki
Published: Case Reports in Psychiatry
The Cunningham Panel™ helps identify an infection-triggered autoimmune encephalopathy in a child initially diagnosed with schizophrenia.
Dr. Shimasaki:
There was a case of a patient diagnosed with schizophrenia. A 15-year-old girl who was treated and in and out of treatment facilities.
Visual:
She was originally diagnosed and treated unsuccessfully for schizophrenia, psychosis, severe anxiety and depression. A more in-depth history revealed that she had an abrupt onset of symptoms with remote acute infections exhibited many characteristics of obsessive compulsive disorder (OCD) with rituals.
Dr. Shimasaki:
But her symptoms were uncontrollable. The physician referred her to an immunologist. And the immunologist knew about our testing and submitted a blood sample for us to test.
Visual:
She had acute onset of “seizure-like spells,” psychotic thinking, and seemingly schizophrenia symptoms, manifesting as auditory hallucinations and catatonic movements.
Dr. Shimasaki:
The patient was positive and began using immunomodulatory therapy.
Visual:
She was able to be weaned off of olanzapine and resume many of her normal activities, including tennis within 2 weeks after plasmapheresis.
Dr. Shimasaki:
And within a few weeks, this patient, a 15-year-old girl who was diagnosed with schizophrenia, in and out of treatment facilities was back home normal and playing tennis and off of all psychiatric medications.
Visual:
After 1 course of plasmapheresis was administered (7 treatments every other day), the patient had complete resolution of her psychotic, OCD and anxiety symptoms.
This is dramatic. All these cases may not be so dramatic but the take home message is that once the underlying root cause can be identified, then clinicians can treat the underlying root with the proper medications.
This study was published in a peer-reviewed journal and there are many more [cases] like this.
The authors describe the case of a 15-year-old female who was initially diagnosed and treated unsuccessfully for schizophrenia, psychosis, severe anxiety, and depression.
At age 15, the patient required 4 inpatient psychiatric hospitalizations due to “an acute onset of “seizure-like” spells, psychotic thinking, and seemingly schizophrenic symptoms, manifesting as auditory hallucinations and catatonic movements.”
Her physical symptoms included dysphonia, mouth twitches, echolalia, frequent pacing, frequent cussing, holding her breath, repeatedly asking the same questions, crying and laughing for no reason, staring, outstretching of her arms for 30 minutes, stumbling, worsening dysgraphia, unable to solve math problem, and worsening reading skills.
The patient was treated unsuccessfully with several antipsychotic medications, including one for severe treatment-resistant schizophrenia.
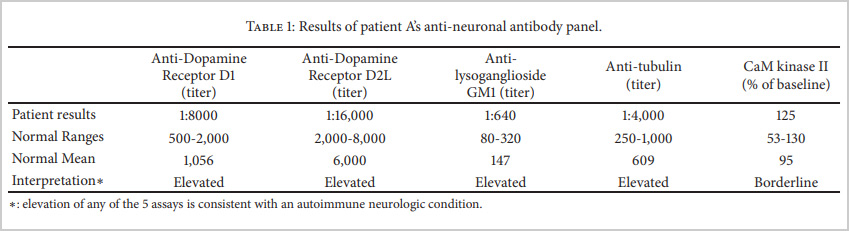
The patient was referred to an immunologist who ordered the Cunningham Panel™. The results indicated a significant elevation of the four autoantibodies and a borderline increase for CaM KII.
“A work-up for underlying infectious, immunodeficiency, and autoimmune causes was unrevealing,” the authors state, “except for very high levels of anti-neuronal antibodies [as measured with the Cunningham Panel] which have been linked to Pediatric Acute-onset Neuropsychiatric Syndrome (PANS).”
“It was decided that plasmapheresis to remove the anti-neuronal antibodies would be most appropriate treatment,” the authors stated.
The patient was treated with one course of plasmapheresis, which led to a complete resolution of her psychotic, OCD, and anxiety symptoms.
She was able to stop the antipsychotic medication and within 2 weeks after stopping plasmapheresis, the patient was able to resume many of her normal activities including tennis.
Authors conclusion:
“This case illustrates the importance of establishing a broad differential diagnosis
including underlying autoimmune encephalopathy, PANDAS/PANS, infection, and other immunologic disorders when evaluating patients presenting with OCD with rituals, severe anxiety, and psychotic symptoms.”
Furthermore, it demonstrates “the importance of exploring nontraditional treatments for severe, treatment-resistant mental illness which requires a multidisciplinary approach.”
Learn More About PANS & Pandas and The Cunningham Panel™

PANS: Diagnosis and Treatment

Pandas & PANS Patient Stories