Syndrome
Autoimmune based chronic fatigue
“In a subset of patients, ME/CFS [chronic fatigue syndrome] begins with infectious mononucleosis and evidence for a potential role of EBV in ME/CFS comes from many studies.” 1 In fact, Epstein–Barr virus and enterovirus are the two most common infectious triggers of CFS. 2
Furthermore, enteroviruses, such as coxsackie, cytomegalovirus (CMV), hepatitis C, Chlamydia pneumonia, and Coxiella burnetii have also been linked with chronic fatigue syndrome. 3 Upper respiratory infections, along with varicella-zoster virus, which causes chickenpox and shingles, have been implicated, as well. 4
ME/CFS may be a variant of an autoimmune disease, writes Fluge et al. “It may involve antibodies, is often triggered by infections, and probably involves a genetic predisposition.” 5
Other studies have also suggested that infection-induced autoimmunity could be a possible disease mechanism. 5
Infections ignite an autoimmune attack
In response to an infection, the body’s immune system produces antibodies. Normally, the antibodies attack and kill any harmful outside substance (i.e. germ, bacteria). But in a subset of patients, these “autoantibodies” mistakenly attack healthy cells (or neurons) within the brain.
“Autoantibodies against various antigens including neurotransmitter receptors have been recently identified in ME/CFS individuals by several groups, and infection by various pathogens … are known as triggers of [the] disease.” 1
This autoimmune attack causes inflammation in the brain and a range of symptoms, including extreme fatigue, brain fog, and other ME/CFS manifestations.
It is well-recognized that inflammation plays a role in Chronic Fatigue Syndrome. A study utilizing PET scans showed chronic fatigue syndrome patients had inflammation in specific regions of the brain (i.e., thalamus and amygdala), which the authors suggest could induce cognitive impairment and severe fatigue. 6
“In the majority of ME/CFS cases, there is no conclusive evidence for chronic viral infection, but it is plausible that viruses could act via a “hit and run” mechanism.” 8
“This theory proposes that viruses trigger the disease, cause immune abnormalities and leave a dysfunctional immune system and/or autoimmunity.” 8
While the causative agents and disease mechanisms may vary, researchers agree there is strong evidence that chronic fatigue syndrome “is associated with a range of biological abnormalities, most notably in the neuroendocrine, autonomic, neurological, bioenergetic, redox and immunological domains.” 9
- https://www.sciencedirect.com/science/article/pii/S1568997218300880 Franziska Sotzny, Julià Blanco, Enrica Capelli, Jesús Castro-Marrero, Sophie Steiner, Modra Murovska, Carmen Scheibenbogen. Myalgic Encephalomyelitis/Chronic Fatigue Syndrome – Evidence for an autoimmune disease, Autoimmunity Reviews. Volume 17, Issue 6, 2018, Pages 601-609.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2921262/ Zhang L, Gough J, Christmas D, et al. Microbial infections in eight genomic subtypes of chronic fatigue syndrome/myalgic encephalomyelitis. J Clin Pathol. 2010;63(2):156–164.
- https://www.frontiersin.org/articles/10.3389/fped.2019.00059/full Kerr, J. Epstein-Barr Virus Induced Gene-2 Upregulation Identifies a Particular Subtype of Chronic Fatigue Syndrome/Myalgic Encephalomyelitis. Front. Pediatr. 13 March 2019.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6702656/ Blomberg J, Rizwan M, Böhlin-Wiener A, et al. Antibodies to Human Herpesviruses in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Patients. Front Immunol. 2019;10:1946.
- https://www.ncbi.nlm.nih.gov/pubmed/26132314 Fluge Ø, Risa K, Lunde S, et al. B-Lymphocyte Depletion in Myalgic Encephalopathy/ Chronic Fatigue Syndrome. An Open-Label Phase II Study with Rituximab Maintenance Treatment. PLoS One. 2015;10(7):e0129898.
- http://jnm.snmjournals.org/content/early/2014/03/21/jnumed.113.131045.abstract Yasuhito Nakatomi, Kei Mizuno, Akira Ishii, Yasuhiro Wada, Masaaki Tanaka, Shusaku Tazawa, Kayo Onoe, Sanae Fukuda, Joji Kawabe, Kazuhiro Takahashi, Yosky Kataoka, Susumu Shiomi, Kouzi Yamaguti, Masaaki Inaba, Hirohiko Kuratsune, and Yasuyoshi Watanabe. Neuroinflammation in Patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: An 11C-(R)-PK11195 PET Study. J Nucl Med. 2014 jnumed.113.131045 published ahead of print March 24, 2014.
- https://www.ncbi.nlm.nih.gov/pubmed/30567628 Russel A. et al. Persistent fatigue induced by interferon-alpha: a novel, inflammation-based, proxy model of chronic fatigue syndrome. Psychoneuroendocrinology. 2019 Feb;100:276-285.
- https://translational-medicine.biomedcentral.com/articles/10.1186/s12967-018-1644-y Rasa, S. et al. Chronic viral infections in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). Journal of Translational Medicine. volume 16, Article number: 268 (2018).
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6428797/ Morris G, Maes M, Berk M, Puri BK. Myalgic encephalomyelitis or chronic fatigue syndrome: how could the illness develop?. Metab Brain Dis. 2019;34(2):385–415.
Learn more about how infections can trigger neuropsychiatric symptoms

Cunningham Panel™ helps identify an autoimmune disorder in child initially diagnosed with schizophrenia
Researchers describe a complex case involving a 15-year-old girl, who abruptly developed multiple neurologic and psychiatric symptoms.
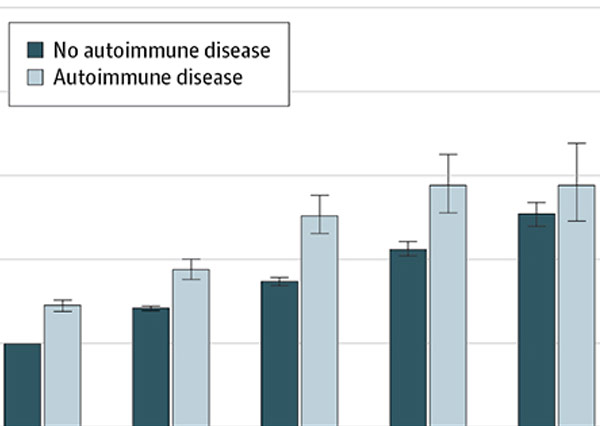
Autoimmune diseases and severe infections as risk factors for mood disorders: a nationwide study
This nationwide, population-based, prospective cohort study examines the link between mood disorders, infections, and autoimmune disease.

Childhood infections can increase risk of mental illness in kids
Nationwide study finds both mild and severe infections can increase risk of mental disorders in children and adolescents.